In Depth: How the WHO’s Global Health Emergency Decision Unfolded

 |
|
|
This is the second part of Caixin’s exclusive four-part in-depth report on China’s fight against the coronavirus outbreak. Please click here to check out part 1 and part 3.
The World Health Organization (WHO) isn’t quick to declare global public health emergencies. From 2007 through 2019, the United Nations group did so on only five occasions. The rapidly spreading new coronavirus that originated in December in China makes a sixth.
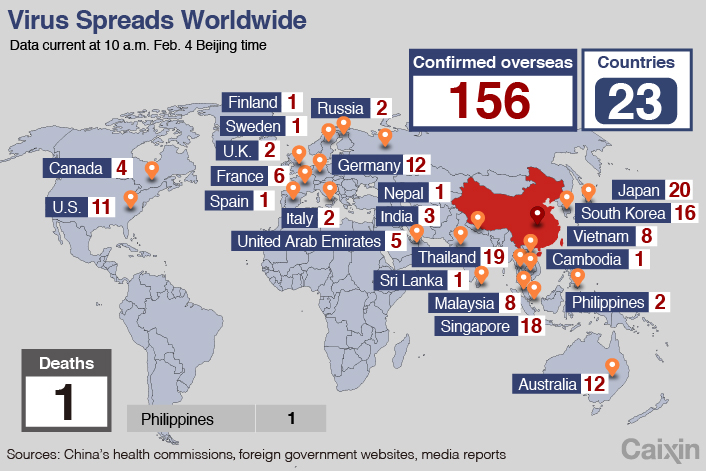
The fallout from the organization’s Jan. 30 call has spread rapidly. Four days later, the total of countries placing border restrictions on Chinese travelers has surged to 60. They include Australia, India, Indonesia, Singapore, New Zealand, Russia and North Korea, and many countries have evacuated or are attempting to evacuate their citizens from Hubei province at the epidemic’s epicenter.
“Our greatest concern is the potential for the virus to spread to countries with weaker health systems” than China’s, WHO Director-General Tedros Adhanom Ghebreyesus said in a tweet. “I am declaring a public health emergency of international concern … not because of what is happening in China, but because of what is happening in other countries.”
The new coronavirus known as nCoV-2019 can lead to severe and often deadly pneumonia. Even as the number of infections and deaths rapidly mounted in Hubei’s capital Wuhan and cases appeared in a growing number of other countries, the WHO took a deliberate approach to evaluating the danger. The body’s emergency committee in meetings Jan. 22-23 initially decided not to designate it a global crisis pending collection of more data.
A week later, the WHO declared the coronavirus the first global public health emergency originating in China. Such a designation didn’t apply to even the SARS epidemic of 17 years ago. A look at how the organization reached its decision shows some of the inner workings of the global system for preventing and managing the spread of dangerous new diseases.
The system relies on the rapid sharing of information among national health systems and the global public health organization. Although some Chinese officials have drawn criticism internally and abroad for initially trying to downplay the crisis, the WHO’s Tedros maintains China was quick to share information, enhancing the global response.
“In many ways, China is setting a new standard for outbreak response,” Tedros said at a press conference. “We would have seen many more cases outside China by now, and probably deaths, if not for the government’s efforts."
Data from China on the pathogen allowed Japan, South Korea and Thailand to diagnose similar cases quickly, Tedros said. For example, a Chinese laboratory warned the German government of an infected person returning to Germany, he said.
Tedros, an Ethiopian public health expert, arrived Jan. 27 in Beijing to meet with Chinese officials. During his visit, Chinese President Xi Jinping called on the country to be transparent in working with the rest of the world and agreed to allow the WHO to send a group of international experts into the country to study the new strain of coronavirus alongside Chinese counterparts.
Those data-gathering steps helped fill the information gap that kept the WHO’s emergency panel from issuing its global warning sooner. Before the Jan. 22-23 meetings, the lack of information on the virulence, infectiousness, severity and clinical symptoms of the coronavirus made reaching a consensus difficult, WHO emergency committee member John Mackenzie told Caixin.
The global organization had evidence of transmission of the virus within a household, but that isn’t unusual for a respiratory disease. The experts were looking for “third- or fourth-generation infections,” referring to how many times a disease has been passed on, an indication of virulence. That evidence came quickly, laying the groundwork for the emergency committee to issue is global warning.
Some argue that compared with the 2003 SARS crisis the Chinese government has been much more transparent about the current coronavirus.
"Before we start pointing the finger at China, we need to recognize there are genuine sensitivities around sharing data around new diseases,” said Mike Ryan, director of the WHO’s health emergencies program who accompanied Tedros to Beijing. “I believe in this case the countries that have been affected, including China, have been remarkably transparent.
According to U.S. Health and Human Services Secretary Alex Azar, China’s compliance with international health regulations and uploading of the genetic sequence of the virus enabled the Americans to develop a test kit to screen for infections.
Weighing the designation
Under the WHO-administered International Health Regulations, a global public health emergency applies to “an extraordinary event which is determined to constitute a public health risk to other states through the international spread of disease and to potentially require a coordinated international response.”
Since 2007, the WHO has declared public health emergencies in response to the 2009 H1N1 influenza pandemic, the 2014 setbacks in global polio eradication efforts, the 2014 West Africa Ebola epidemic, the 2016 Zika virus outbreak and the 2018-2019 Kivu Ebola epidemic.
The organization’s emergency committee, which makes the call, is made up of epidemiologists, virologists and infectious disease experts appointed by the WHO secretary-general. Among them, at least one expert comes from the country where the epidemic began. The panel can also make recommendations to foreign governments on measures such as travel or trade restrictions.
Even during serious crises, the WHO is conservative in its pronouncements. Through July last year, the Kivu Ebola epidemic killed 1,500 and infected more than 2,300 after appearing in the Democratic Republic of the Congo in August 2018 and spreading to nearby countries. The disease wasn’t declared an international public health emergency until the WHO’s fourth emergency committee meeting in July 2019.
Three factors weighed on the current WHO decision, according to Didier Houssin, chairman of the WHO emergency committee. They were the rising number of cases in China, the growing number of countries with confirmed infections and the spread of questionable measures by some nations involving travelers.
While the emergency committee doesn’t encourage travel or trade restrictions, it acknowledges that such steps can be useful at times, such as when response capabilities are limited or when there’s a large likelihood of infection among vulnerable groups.
Under the International Health Regulations, countries are required to report travel restrictions to the WHO, and they are barred from taking steps that encourage discrimination.
Foreign reactions
 |
After news broke of the coronavirus that originated in Wuhan, many countries imposed increasingly stringent measures. In addition to posting travel warnings and tightening border controls, several counties implemented preliminary screening measures using their own public health organizations to diagnose those who may have come into contact with the virus even before they showed symptoms.
The U.S. reacted especially quickly. On Jan. 17, four days after Thailand reported its first case, the Centers for Disease Control and Prevention (CDC) said it would screen passengers arriving from Wuhan at major airports in New York, Los Angeles and San Francisco. At the time, the U.S. had not reported any cases of the disease. After it did so, the country expanded screenings of Chinese passengers to 20 airports while also advising against all travel to China.
On Friday, the U.S. declared the coronavirus epidemic a public health emergency and temporarily closed its borders to foreign nationals who traveled to China in the previous two weeks and weren’t immediate family members of U.S. citizens or permanent residents. The government also imposed mandatory two-week quarantines for those who were in China’s Hubei province during that time span.
As she confirmed Europe’s first case of nCoV-2019 on Jan. 24, the French health minister Agnes Buzyn promised total transparency and daily updates to combat misinformation. She said sharing epidemic information with the public was the best barrier to its spread.
International response
 |
Even though China shared the virus’s genome sequence Jan. 11, researchers don’t yet have a full grasp of its characteristics and routes of transmission, according to the WHO.
Because developing a vaccine or treatment requires significant time and resources, all countries — including China and the U.S. — should pool their efforts, said Richard Hatchett, chief executive of the Coalition for Epidemic Preparedness Innovations (CEPI), an international epidemiology group.
CEPI, made up of public and private entities, said Jan. 23 that it was funding research into three separate efforts to develop a vaccine for the nCoV-2019 virus with the aim of shortening development time to several months.
The U.S. National Institutes of Health received the virus’s genetic sequencing and started research on vaccines, Anthony Fauci, director of the U.S. National Institute of Allergy and Infectious Diseases, told CNN Jan. 20. He cautioned that the development process can last months or years, so controlling the epidemic will require “traditional” public health measures.
So long as there is no vaccine, the only available measures for slowing the spread of the disease are quarantine, delaying resumption of work and schools, and restricting travel, Hatchett said last month at the World Economic Forum in Davos, Switzerland. He cautioned that the cost of these measures is high and difficult to sustain.
From studying nonmedical interventions in the 1980s, the U.S. found that disease prevention is more effective when a city implements various interventions during the onset of an outbreak, Hatchett said. As a U.S. government public health official in 2005, Hatchet helped draft the country’s epidemic response plan in light of the outbreak of the H5N1 influenza.
Xu Heqian, Wu Hongyuran, Qu Yunxu, Zhang Qi, Chen Lixiong and Li Xin contributed to this story.
Contact reporter Dave Yin (davidyin@caixin.com) and editor Bob Simison (bobsimison@caixin.com).

- MOST POPULAR





