In Depth: Why South Korea Is Winning Its Covid-19 Fight

 |
South Korea’s coronavirus outbreak once looked grim with new cases skyrocketing on a daily basis and a massive cluster of infections, making it the worst-hit country outside China.
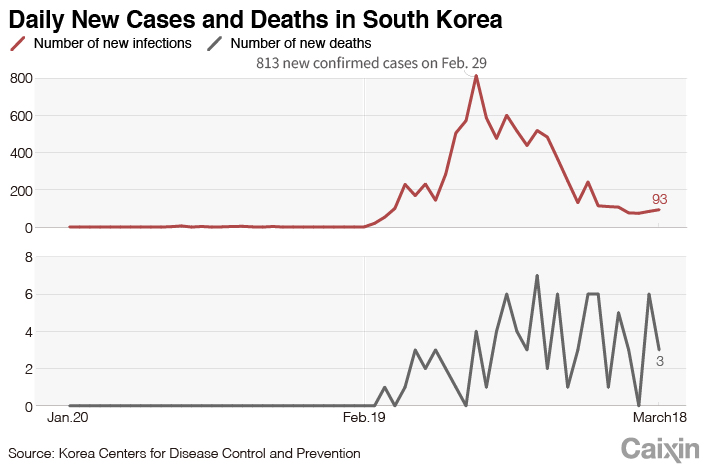
The disease suddenly exploded in South Korea Feb. 18. The caseload multiplied 180-fold in two weeks, with daily growth topping 909 on Feb. 29. But the dire trend reversed course quickly. Since March 6, South Korea started reporting declining numbers of new cases with daily increases in the dozens. As of Sunday, South Korea recorded 8,897 infections, No. 8 in the world.
Elsewhere, the Covid-19 pandemic only grows more dreadful over time. In the United States, where the first case was detected Jan. 20, the same day as South Korea’s, total infections exceeded 32,000 by Sunday afternoon, with at least 389 deaths. In Spain, total caseload reached 28,603, adding more than 3,600 overnight. In Italy, the new hotspot of the outbreak, infections surpassed 59,000 with more than 5,400 fatalities.
Globally, more than 320,000 people have contracted Covid-19, and 14,000 people have died, according to Johns Hopkins University. To stop the spread of the virus, an increasing number of governments are turning to draconian measures from city shutdowns to sealing borders.
But South Korea showed there is another way to effectively bring the disease under control. Businesses across the country have largely carried on, and no city was locked down. With falling numbers of new cases, life in South Korea seems to be on track to returning to normality.
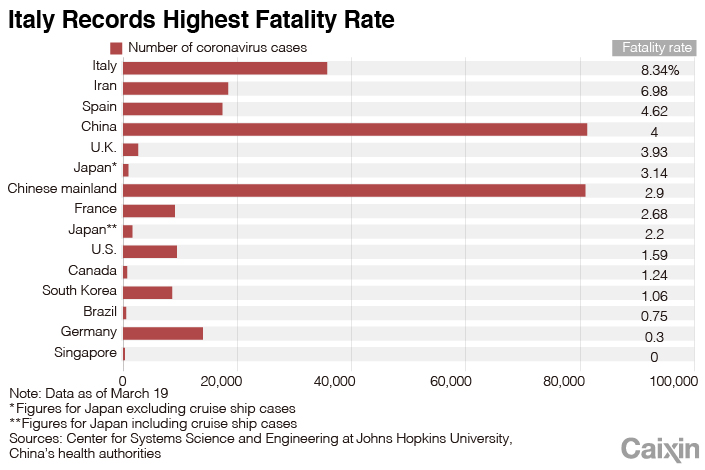
More importantly, South Korea has one of the world’s lowest fatality rates from Covid-19 at just 1%, compared with the 3.4% global fatality rate estimated by the World Health Organization in early March.
Korean officials attribute to the country’s effective control of the outbreak to a strategy called TRUST, for transparency, robust screening and quarantine, unique but universally-applicable testing, strict control and treatment.
South Korea learned the importance of preparedness the hard way in the face of an epidemic after the 2015 outbreak of Middle East respiratory syndrome (MERS). A single imported case of MERS set off a chain of transmission that infected 186 and killed 36. Nearly 17,000 people were quarantined, and the government was harshly criticized for its slow response.
As Covid-19 cases emerged in China late last year, South Korea started mobilizing resources for an outbreak. The country tested people for the virus at the fastest pace in the world, enabling early detection of patients, effective isolation and timely treatment to reduce mortality.
Its invention of drive-through test stations, which allow people to take swabs to test for the virus without leaving their cars, is now being copied by countries including Canada, Germany and the U.S.
 |
According to government data, South Korea has the ability to test an average of 12,000 people a day with peak capacity of as many as 20,000 a day. People usually receive test results within six to 24 hours. As of Friday, South Korea tested more than 300,000 of its 51 million people, or more than one of every 200.
By contrast, the U.S., with a population more than six times that of South Korea, may have tested only about 170,000 people, according to Dr. Deborah Birx, a member of the White House Coronavirus Task Force.
“The South Korean government responded quickly and took effective measures after the emergence of super-spreaders,” said Huang Yanzhong, a public health researcher at the U.S. Council on Foreign Relations. Massive testing is an important factor for stopping the virus and played a decisive role in controlling the epidemic at an early stage, Huang said.
Even though the country reported 152 new cases Thursday with the emergence of new clusters over the past week, South Korea's handling of the outbreak is a model of early action and swift containment, experts said. A look at the country’s path over the past two months may provide lessons for other countries.
Early reaction
News of an unknown pneumonia emerging in Wuhan in central China came to light around Dec. 31. Three days later, the Korea Centers for Disease Control and Prevention (KCDC) set up an emergency team to study the disease.
On Jan. 8, South Korea reported its first suspected case — a 36-year-old Chinese from Gyeonggi Province who visited Wuhan in mid-December. The patient, who showed pneumonia-like symptoms, later tested negative for coronavirus, but the incident sounded the first alarm to the country.
Read more
Caixin’s coverage of the new coronavirus
South Korean authorities stepped up efforts starting Jan. 16 to screen people who had visited Wuhan as cases of infection were reported in Thailand and Japan.
The first case was confirmed Jan. 20 and reported to the public, the same day Beijing and Guangzhou reported their first cases. The KCDC immediately raised its alert level. At the same time, authorities started tracking health conditions of about 3,000 people who had traveled to Wuhan over the previous 14 days, and lawmakers moved to revise laws to assist in disease control efforts.
Following Wuhan’s lockdown Jan. 23, the KCDC dispatched an expert team to the city to study the outbreak. Meanwhile, construction of a massive virus-testing network started in South Korea in a joint effort of private and public institutions. It went into operation in early February.
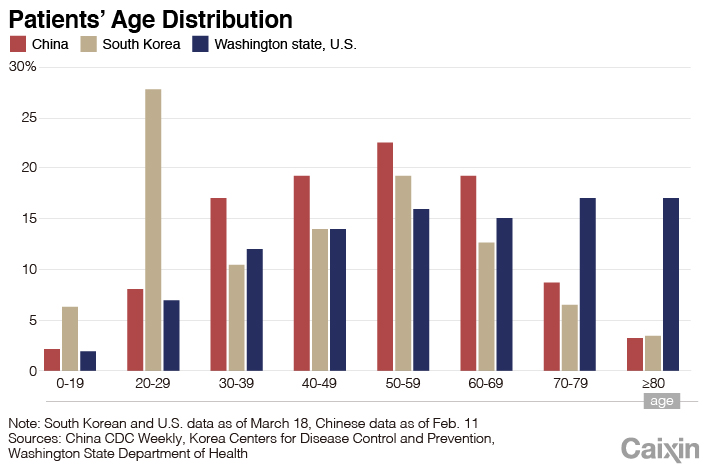 |
The Covid-19 outbreak is the first major test for South Korea’s disease control system since an overhaul triggered by the 2015 MERS outbreak. The revamp gave the KCDC greater authority in handling epidemics and equipped hospitals with adequate quarantine and pathogen testing facilities.
The system proved effective. In the month after South Korea’s first confirmed case, the daily increase in infections remained fewer than four, and no cases were reported between Feb. 12 and 15. As of Feb. 16, the total reached 30 infections, including 14 inbound travelers and 16 of their close contacts. On Feb. 18, President Moon Jae-in predicted the outbreak would “disappear before long.”
He spoke too soon. The next day, South Korea reported a record of 20 new cases, including 14 linked to a religious group known as the Shincheonji Church of Jesus in Daegu, the country’s third-largest city after Seoul and Busan.
The previous day, South Korea diagnosed its 31st patient with Covid-19, a person who soon became known as the country's "super-spreader." The 61-year-old woman, who did not travel abroad since December, was part of the mass congregation of the Shincheonji Church and came in contact with more than 1,000 people.
 |
Medical workers transport a Covid-19 patient in Seoul March 8. |
On Feb. 20, South Korea added 53 new cases, more than the total count over the previous month. Of the new infections, 23were linked to Patient 31. Since then, new cases surged every day, and the total number more than doubled in the week between Feb. 29 and March 7.
It is still unclear who was the first patient in the Shincheonji Church, but the organization’s intensive network of 210,000 members nationwide allowed the virus to spread at lightning speed. On Feb. 25, the government started to screen all Shincheonji Church members. As of March 3, 13,241 members reported suspected symptoms. In Daegu, 4,328 members received tests, and 62% were positive.
On March 3, President Moon declared war on the outbreak.
 |
Get tested
Song Qiao, a Chinese woman in South Korea, received a notice from a community clinic asking her to stay in self-isolation after one of her friends at the Shincheonji Church was confirmed with the infection. During her quarantine, Song received daily calls from the clinic inquiring about her condition. Several days later, she was tested for the virus and had a negative result.
“The South Korea government acted quickly in tracing and testing suspected patients,” Song said. “When one case is confirmed, all people and places that had contact with the patient are traced.”
Since the outbreak, South Korea has established 118 labs and 633 testing sites, including drive-through clinics and pop-up facilities, forming an intensive network to provide fast and affordable public testing. In two weeks since the outbreak escalated in late February, 120,000 people in South Korea were tested.
Jin Yong Kim, a Korean infectious disease physician, said the country’s decision to conduct massive testing effectively suppressed the highly infectious virus. With large-scale screening, early treatment and quarantine measures can be carried out in a timely way, he said.
Compared with the MERS outbreak, when contagion mainly took place in hospitals, Covid-19 has greater risk for community transmission. South Korea’s authorities quickly realized the difference and shifted the control strategy to mass testing, Kim said.
South Korea was well prepared for the shift. When Chinese scientists first published the novel coronavirus's genetic sequence in January, South Korean companies started developing and stockpiling test kits, even before the country had its first case.
The government approved its first test kit Feb. 4, made by Seoul-based Kogene Biotech Co., when the country had reported just 16 cases. According to Korean media reports, as of March 16, four Korean companies won approval to produce test kits and started mass production. Their total capacity has met domestic demands, and the manufacturers say they plan to seek exports.
“South Korea’s experiences showed how a sound coordination between the state and private sector can benefit efforts to screen and contain the disease,” said Huang at the U.S. Council on Foreign Relations.
Massive testing is the key that helped South Korea control the outbreak and reduce fatalities, said Stanley Perlman, professor of microbiology and immunology at the University of Iowa. But such measures could be carried out partly because of South Korea’s relatively small territory and will be a challenge for large countries like China and the U.S., Perlman said.
South Korea also adopted rigorous quarantine measures to prevent the virus’s spread. Such measures grew out of the painful lessons of Daegu, which has nearly three-quarters of all cases in the country.
As in the early days in Wuhan, hospitals in Daegu were overwhelmed, resulting in high mortality because of delayed treatment, local epidemiologists said. Meanwhile, many mild patients were told to stay in home quarantine, causing clusters of infections among family members.
On March 1, Daegu had 2,569 confirmed patients. But only 898 of them were hospitalized and the rest were at home. The same day, the South Korean government issued new guidance for Covid-19 including setting up designated facilities to receive patients at different phases of the disease to reduce the burden on hospitals, similar to the idea of makeshift hospitals in Wuhan.
Since then, hotels and company dormitories were reserved as makeshift wards and quarantine sites to put mild and suspected patients under centralized observation.
Mass testing and strict quarantine measures allowed South Korea to slow the outbreak without shutting down cities and banning travel. Despite social and cultural differences, South Korea’s epidemic control measures can be implemented in other parts of the world, said Jeremy Rossman, a virologist at the University of Kent.
Unfinished war
The battle against a global pandemic can hardly rely on one country by itself. On March 13, China and South Korea formed a joint task force to control Covid-19 with coordination of customs, disease control and treatment research. Four days later, Japan joined the partnership.
While the outbreak in the earliest-hit Asian countries showed signs of waning, experts warned it is too early to relax as the risks of new infections linger.
South Korea maintained its downward trend of new cases starting March 7 with daily increases of fewer than 100. That ended, however, with a rebound March 19, when 152 new infections were reported, including a cluster of infections at a nursing home in Daegu. The previous week, another cluster of cases appeared around a call center in Seoul.
The emergence of new clusters and unknown infection sources indicates that there is undetected community transmission, said Chun Byung-Chul, an epidemiologist at Korea University in Seoul.
“As long as there are still uncertainties, we can’t say the outbreak has peaked,” Chun said.
South Korea has stepped up measures to address the potential revival of the epidemic. Since March 16, the country started screening all people arriving at airports, Koreans included.
The spread of Covid-19 has been slowed in South Korea and China largely because of the implementation of strict social distancing and public hygiene, said physician Jin.
“It won us a precious time to review our efforts to prepare for the new outbreak,” Jin said. "The enemy we fear most is not the virus, but the next surge we must face without changing our current lifestyle."
Contact reporter Han Wei (weihan@caixin.com) and editor Bob Simison (bobsimison@caixin.com)

- MOST POPULAR







